Before attending an oral surgery consultation in Anaheim, patients should meticulously prepare by formulating pertinent questions. Evaluating the surgeon’s credentials, including their board certification and experience, is essential. An understanding of anesthesia options and their risks is equally important. In addition, comprehending the surgical process, recovery timeline, and post-operative care is crucial. Clarifying costs and insurance coverage guarantees transparency. Addressing these aspects will empower patients, equipping them with the knowledge needed for informed decision-making.
Understanding the Procedure
Understanding the specific details of an oral surgery procedure is essential for patients to make informed decisions about their healthcare. The procedure details involve a thorough explanation of each step, from pre-operative preparations to post-operative care, ensuring alignment with patient expectations. Clinicians should provide a detailed overview of the surgical process, including anesthesia options, duration, and recovery time. Additionally, potential risks and complications must be clearly communicated to prepare patients adequately. This transparency enables patients to anticipate their role in pre-surgery preparations and post-surgery recovery, fostering realistic patient expectations. By understanding the procedure details, patients can engage proactively in discussions with their healthcare provider, ultimately leading to more satisfactory outcomes and a well-informed surgical experience.
Evaluating the Surgeon’s Experience
When considering oral surgery, how does one effectively evaluate the surgeon’s experience? A critical step involves examining the surgeon’s qualifications. Prospective patients should verify board certification, which indicates adherence to rigorous professional standards. In addition, inquire about their educational background and specialized training in oral surgery. Another significant aspect is the surgeon’s surgical success rate. Reviewing statistics related to past procedures, complication rates, and patient outcomes provides insight into their proficiency. Moreover, testimonial reviews and peer recommendations can offer qualitative data on the surgeon’s expertise. It is paramount to assess the number and variety of surgeries performed, as extensive experience correlates with higher competency. Thoroughly evaluating these factors guarantees informed decision-making, thereby optimizing surgical outcomes and patient safety.
Discussing Anesthesia Options
When preparing for oral surgery, understanding the anesthesia options is vital for patient safety and comfort. Patients should inquire about the types of anesthesia available, such as local anesthesia, sedation, or general anesthesia, and discuss which option best suits their medical history and procedure requirements. Additionally, it is important to address any anesthesia safety concerns, including potential side effects and the qualifications of the anesthesia provider, to guarantee a thorough understanding of the risks involved.
Types of Anesthesia Available
How essential is it to understand the various types of anesthesia available for oral surgery? Comprehending the distinctions among anesthesia types is vital for patients undergoing oral procedures. Local anesthesia is commonly administered to numb a specific area of the mouth, ensuring that the patient remains awake and alert while minimizing discomfort. This option is typically used for less complex procedures such as tooth extractions or fillings. On the other hand, general anesthesia induces a state of unconsciousness, allowing the patient to be completely unaware of the procedure. This is often reserved for more extensive surgeries, where patient immobility and comfort are paramount. Understanding these options enables informed decision-making, aligning patient comfort with the procedural requirements and the surgeon’s recommendations.
Anesthesia Safety Concerns
Understanding the types of anesthesia is only part of the preparation for oral surgery; evaluating anesthesia safety concerns is equally important. Anesthesia types vary markedly, with general anesthesia, local anesthesia, and intravenous sedation being most prevalent. Each type carries distinct safety profiles and risks, necessitating thorough discussion with the oral surgeon. Sedation levels, ranging from minimal conscious sedation to deep sedation, should be carefully considered based on the patient’s medical history and the complexity of the procedure. A thorough preoperative evaluation is essential, including a review of the patient’s allergies, current medications, and any previous anesthesia reactions. This assessment helps mitigate potential complications, ensuring that the chosen anesthesia type and sedation level align with the patient’s health status and procedure requirements.
Exploring Potential Risks and Complications
Prior to undergoing oral surgery, it is imperative for patients to understand the common surgical risks, which may include infection, bleeding, and adverse reactions to anesthesia. Equally important is the discussion of strategies to effectively manage potential post-surgery complications, such as swelling, pain, and impaired healing. Thorough preoperative consultations can mitigate these risks by equipping patients with essential knowledge and fostering informed decision-making.
Common Surgical Risks
When considering oral surgery, it is essential to examine the potential risks and complications that may arise during or after the procedure. Among the primary concerns are surgical infections, which can occur if bacteria enter the surgical site. This risk necessitates strict adherence to sterile techniques and may require postoperative antibiotic therapy. Bleeding risks are another significant concern; they can arise from incisions, tissue manipulation, or vascular injury. Proper surgical technique and preoperative assessment of clotting function are critical in mitigating these risks. Additionally, patients with pre-existing conditions such as coagulopathy may require special precautions. Understanding these common surgical risks allows for informed decision-making and thorough discussions with the oral surgeon, ensuring patients are well-prepared for their procedure.
Managing Post-Surgery Complications
Addressing the potential risks during oral surgery forms the foundation for effectively managing post-surgery complications. A thorough understanding of potential complications, such as infection, swelling, or prolonged bleeding, is essential. Implementing robust pain management strategies is critical to patient recovery, utilizing both pharmacological options and non-pharmacological techniques, such as cold compresses. Surgeons are advised to discuss these strategies with patients preemptively to guarantee they are well-prepared. Additionally, scheduling regular follow-up appointments plays a pivotal role in monitoring post-operative progress and early detection of complications. These appointments allow for timely intervention should any adverse symptoms arise, thereby minimizing the risk of long-term issues. Adhering to these protocols considerably enhances patient outcomes and mitigates the impact of potential post-surgical complications.
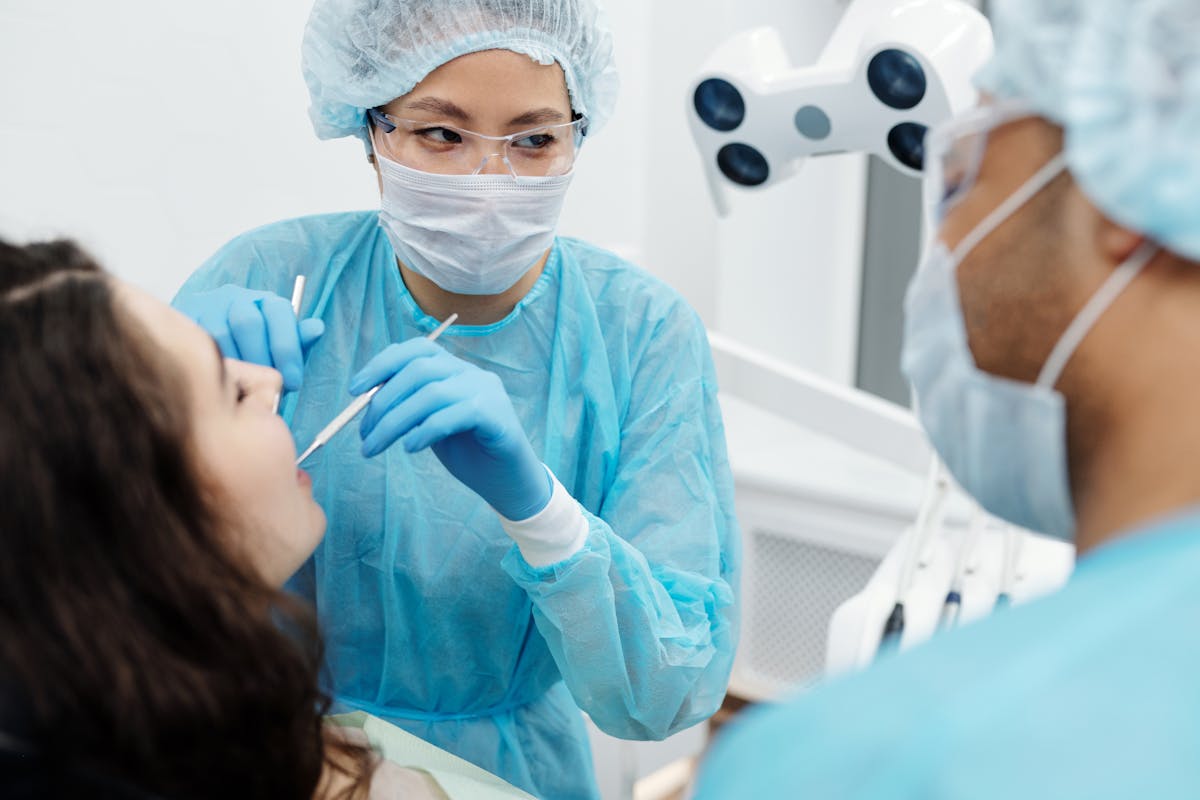
Reviewing the Recovery Process
Understanding the recovery process is essential for patients preparing for oral surgery, as it directly impacts the overall surgical outcome and patient well-being. The recovery timeline varies considerably based on the complexity of the procedure and individual patient factors. Typically, initial healing occurs within the first week, with full recovery spanning several weeks. Effective pain management is critical during this period to guarantee comfort and facilitate healing. Patients should discuss with their surgeon the anticipated duration of discomfort and the prescribed analgesics or alternative pain relief methods available. Additionally, understanding potential postoperative symptoms, such as swelling or limited oral function, helps in setting realistic expectations. A well-informed patient can actively participate in their recovery, contributing to a more favorable surgical outcome.
Clarifying Post-Surgery Care Instructions
A thorough understanding of the recovery process naturally leads to the importance of clarifying post-surgery care instructions. Patients should inquire about post operative expectations to guarantee a smooth recovery. Vital topics include dietary restrictions, activity limitations, and oral hygiene practices. Specific medication guidelines must be addressed, including dosage, frequency, and potential side effects of prescribed analgesics or antibiotics. Understanding these directives will mitigate complications and promote healing. Patients should also confirm emergency contact procedures in case of unforeseen issues. Discussing follow-up appointments to monitor recovery progress is essential. A detailed grasp of these instructions not only aids in adherence but also prepares individuals to manage their recovery effectively, aligning with their surgeon’s recommendations for best outcomes.
Assessing the Timeline for Healing
How long should patients expect the healing process to take after oral surgery? The healing timeline varies considerably depending on the complexity of the procedure, individual health conditions, and adherence to post-operative care instructions. Typically, initial recovery expectations range from 48 to 72 hours for minor procedures, during which swelling and discomfort are most pronounced. However, complete tissue repair and bone integration may extend from several weeks to months. Patients should anticipate follow-up appointments to monitor progress and address any complications. It is crucial to maintain communication with the oral surgeon to adjust recovery expectations based on individual healing responses. By understanding the healing timeline, patients can better prepare for their recovery journey and guarantee ideal outcomes.
Confirming Cost and Insurance Coverage
When contemplating oral surgery, precisely determining the cost and understanding insurance coverage are paramount. Patients should seek a detailed cost breakdown from their oral surgeon in Anaheim, detailing each component of the procedure, from anesthesia to post-operative care. This financial transparency enables individuals to anticipate expenses accurately. Concurrently, reviewing insurance policies is essential to ascertain which aspects of the surgery are covered. Patients should verify with their insurer the extent of coverage, including deductibles and co-payments, and identify any pre-authorization requirements that may be necessary prior to the procedure. By addressing these financial aspects, individuals can make informed decisions, ensuring that both out-of-pocket expenses and insurance contributions are clearly understood before proceeding with their oral surgery consultation.
Addressing Any Personal Concerns or Questions
Before proceeding with oral surgery, patients should meticulously address any personal concerns or questions with their oral surgeon to guarantee a thorough understanding of the procedure. This dialogue is vital for alleviating personal anxiety and guaranteeing a seamless surgical experience. Patients are advised to disclose any previous experiences with surgery that might influence their current apprehensions or expectations. It is essential to inquire about the specifics of the procedure, anticipated recovery time, and potential risks or complications. Understanding these elements thoroughly can mitigate apprehension and foster confidence in the surgical process. Additionally, discussing pain management strategies and postoperative care will help prepare the patient mentally and physically. This proactive approach guarantees that patients are informed and reassured, leading to improved outcomes and satisfaction.
Frequently Asked Questions
What Should I Wear on the Day of My Oral Surgery?
Patients should opt for comfortable clothing and loose fitting attire on the day of oral surgery. This choice facilitates ease of movement, minimizes discomfort, and guarantees accessibility for medical staff during pre-operative and post-operative procedures.
Can I Bring a Friend or Family Member to the Consultation?
Inquiring about the possibility of bringing a support person to the consultation is advisable. Their presence can enhance consultation benefits by providing emotional support, assisting with information retention, and ensuring thorough understanding of the surgical procedure.
How Soon Can I Eat and Drink Before the Surgery?
The patient should adhere to pre-surgery guidelines, which typically involve fasting for a specified period. Hydration recommendations may allow clear fluids up to a certain time before the procedure, ensuring ideal conditions for anesthesia and recovery.
Will I Need to Arrange for Transportation After the Surgery?
Patients typically need to arrange transportation post-surgery due to anesthesia options affecting alertness and coordination. Post-surgery care often includes monitoring recovery and ensuring safety, making it essential for someone else to drive them home after the procedure.
Are There Any Dietary Restrictions Leading up to the Surgery Date?
The inquiry regarding dietary restrictions focuses on pre-surgery nutrition and hydration guidelines. Patients should adhere to specific dietary protocols, such as fasting or consuming clear liquids, to optimize surgical outcomes and minimize complications during oral surgery.
